
Age brings many changes that may affect appetite and the ability to meet the body’s nutritional needs. However, exterior challenges to senior nutrition, such as cost, also exist. Keep reading to learn how to support older adults’ health.
Learn How To Support Senior Nutrition
March is National Nutrition Month, which educates people about the importance of developing healthy habits like eating right and staying active. This month is also an opportunity to support older adults by learning about common challenges to good senior nutrition.
Of course, meeting the body’s nutritional needs is essential for a long and healthy life. But unfortunately, several age-related changes can make doing so easier said than done. For example, appetite loss can make eating less enjoyable, interesting, and important. Over time, regularly missing meals can make it tough to consume enough nutrients and increase the risk of malnutrition.
Barriers To Senior Nutrition Impact Overall Health
Older adults who don’t meet their nutritional needs are more likely to have health complications and extended hospitalizations than those who do. For example, malnutrition in seniors is a serious problem that can cause a range of health problems, such as:
- Fatigue
- Anemia
- Weight loss
- Lower immunity
- Higher risk of falls
- Weakened muscles
- Higher infection risk
- Longer healing times
- Diminished bone mass
Naturally, this means higher costs for individuals and health systems alike. According to a 2020 study, the various diseases linked to malnutrition cost an estimated $147 billion annually, with $15.5 billion associated with direct therapeutic costs.
Unfortunately, many older adults face often face obstacles to maintaining their nutritional needs, such as:
- Loneliness and isolation
- Food costs and limited incomes
- Limited options and transportation
- Physical changes and health problems
Understanding the challenges to senior nutrition below readies family members and caregivers of at-risk loved ones with the knowledge and solutions to overcome them, lowering the impact of poor senior nutrition on overall health.
Age-Related Changes
Several age-related changes can make it difficult to eat or make eating a less enjoyable experience. For example, some prescriptions (and aging) may change smell and taste or reduce appetite altogether. Or, someone with Alzheimer’s or arthritis may no longer be able to cook. Below are more physical changes that hinder senior nutrition.
Appetite Loss
In a 2019 study, 60% of adults 65 and older and 80% of those over 80 reported taste loss. Appetite loss is common with age and can cause people to lose interest in eating. Loss of appetite can also be due to hormone changes. For example, cholecystokinin (CCK) is the hormone that makes us feel full. The body produces more CCK as we age, making seniors feel satiated, even when barely touching their plates.

Appetite loss can also occur due to changing taste buds (sweet and salty foods can get harder to taste) or as a side effect of certain medications. Diminished taste and smell can contribute to general dissatisfaction with eating. Older adults with a reduced taste for sweet and salty foods often crave foods higher in fat and sugar. Of course, this is usually to the detriment of their nutrition.
Swallowing Problems
As mouth and throat muscles weaken with age, swallowing problems (or dysphagia) can make eating certain foods, like meats and fresh vegetables, very difficult. Besides muscle weakness, dysphagia can also occur due to poorly fitted dentures, poor oral health, lower saliva production, and more.
Gastrointestinal Problems
Excessive gas, acid reflux, and other issues in the stomach and intestines can deter seniors from foods that trigger these symptoms. Diminished saliva production can also disrupt digestion after eating. Consequently, they may only sometimes get the necessary vitamins and nutrients, like protein, fiber, and calcium.
Dental Problems
Oral health affects many body functions, including eating. As oral health declines with age, issues such as painful teeth and gums can develop and cause discomfort while eating, discouraging people from eating.
Besides addressing dental issues with a professional as soon as possible, seniors should try foods with different textures and consistencies, such as smoothies, minced vegetables, cottage cheese, and other soft foods.
Loss Of Kidney Function
Age also causes kidney function changes, which affects the body’s ability to regulate water levels. As the kidneys lose their ability to hold fluid, it can cause dehydration, which is especially problematic for older adults who lose their ability to recognize thirst.
Financial Concerns
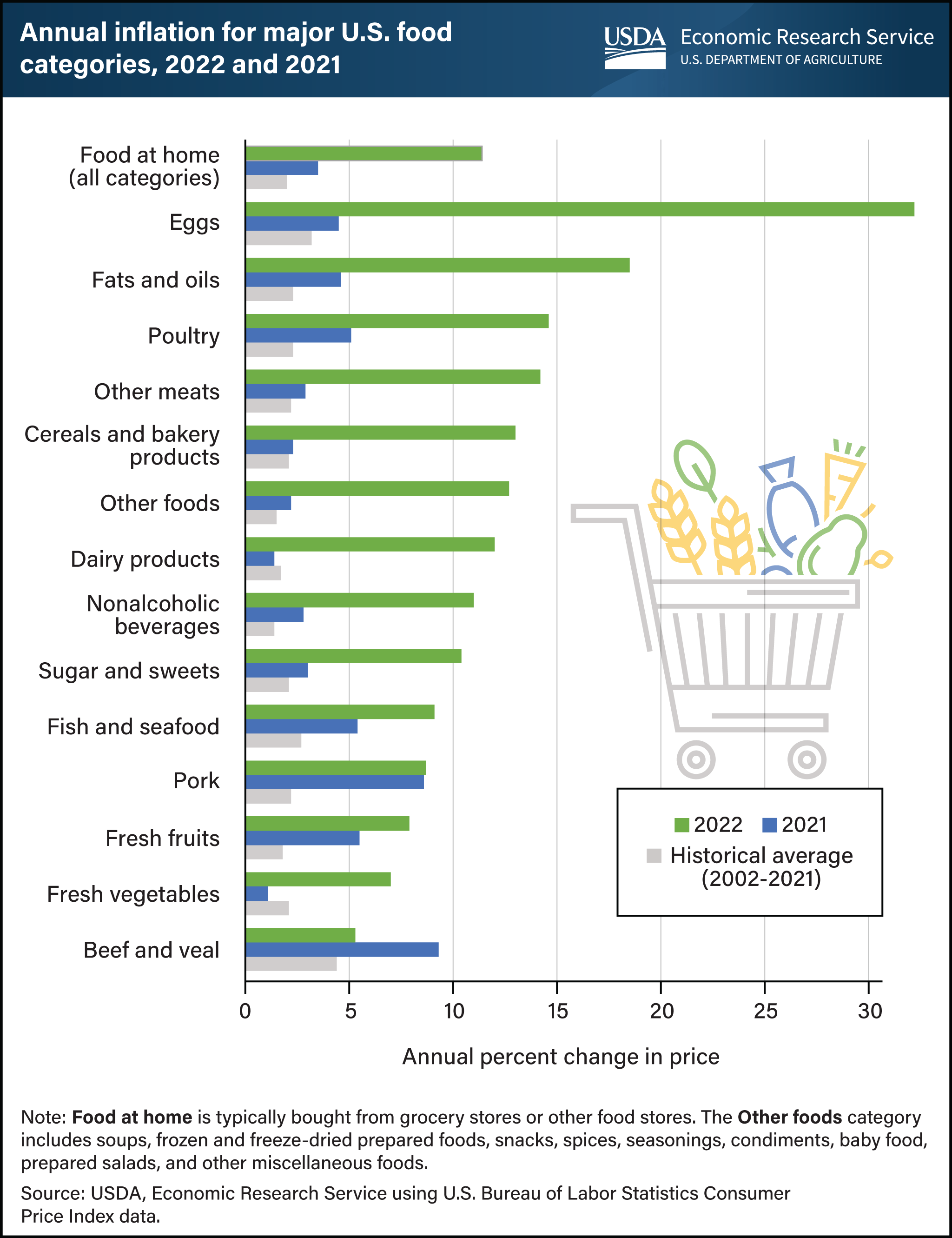
Financially-burdened seniors often reduce or eliminate food or healthy meals due to cost. In 2021, the federal poverty line was $12,880 for individuals and $17,420 for couples. That year, half of US adults over 65 had annual incomes less than $27,382. Meanwhile, food costs have risen to the highest in over 40 years, with grocery store food prices rising 9.9% in 2022.
Transportation Access
Transportation is essential because it ensures access to health services, community programs, and basic services like grocery stores. But unfortunately, many seniors lack access to reliable transportation because they don’t have a vehicle or live in an area with limited public transit options. Or, they may have mobility issues, diminished vision or hearing, or cognitive impairment.
Consequently, elderly adults often depend on relatives, friends, or neighbors for rides. However, this solution isn’t necessarily ideal (or possible) for everyone. Although delivery and pickup options are on the rise, they are only solutions for some.
Loneliness And Isolation
For most people, mealtime is a shared experience. However, those living alone may be less interested in mealtime because they don’t want to eat by themselves. Or, they may feel less motivated to cook because they don’t want to just for themselves.
In addition, loneliness and isolation in seniors can cause appetite loss or deter the desire to cook. These factors increase the risk of malnutrition, so care teams and family members need to recognize the signs of depression in the elderly and address issues sooner rather than later.
Senior Nutrition Programs Can Be Difficult To Access
Senior nutrition assistance from the Supplemental Nutrition Assistance Program (SNAP) and similar organizations are invaluable resources for those in need. However, some older adults may find applying to these programs (and taking the necessary steps to keep their benefits) complex and confusing.
The cost of reaching welfare offices can also deter potential beneficiaries, while some may not apply because of the stigma associated with government assistance. Separately, limited monthly benefits may not offer enough to afford healthier options. For example, average monthly SNAP benefits from October 2019 to September 2020 were $240 for households and $121 for individuals, or $4.00 per day.
Fortunately, experts estimate that in 2023, monthly SNAP benefits will increase to $186 per person ($6.10 per day). Yet, these measures may be insufficient against inflation-fueled food costs, which the United States Department of Agriculture (USDA) projects will rise by 7% in 2023.
Lastly, many local and national organizations, including Meals On Wheels, have reduced deliveries in many communities. Consequently, some recipients may only receive fresh food a few times a month. In some cases, services may only provide frozen meals.
As a “nutritionally-vulnerable” group, older adults have unique food needs to prevent or manage various conditions and diseases. For example, many health professionals recommend foods low in sugar and sodium but high in vitamin D or calcium. However, assistance programs may infrequently have these foods available, which is another barrier to senior nutrition.
List Of Senior Nutrition Programs
Here are a few senior nutrition programs available on the state and national levels:
- Meals on Wheels
- Assistance for Seniors Age 60 and Over
- Child and Adult Care Food Program (CACFP)
- Commodity Supplemental Food Program (CSFP)
- Food Distribution Program on Indian Reservations
- Senior Farmers’ Market Nutrition Program (SFMNP)
- Supplemental Nutrition Assistance Program (SNAP)
- Administration for Community Living: Nutrition Services
- Older Americans Act (OAA) Nutrition Programs Fact Sheet
- Child and Adult Care Food Program (CACFP): Adult Day Care Centers
MeetCaregivers Helps Support Senior Nutrition
National Nutrition Month encourages the public to learn about healthy food choices and the importance of senior nutrition. In addition, older adults, family members, and caregivers should understand the aging body’s changing needs because it will make recognizing and addressing potential barriers to nutrition easier.
If your loved one needs help with cooking, eating, or something else, MeetCaregivers can help. A professional caregiver can help make meals based on a doctor’s plan and help support your loved one’s dietary needs. A caregiver can also ensure seniors aren’t eating expired foods and getting physical exercise in addition to eating right.
For more information, call 1 (888) 541-1137, or find a caregiver today.
Visit our Blog for more resources on aging in place and long-term care.
- Center on Budget and Policy Priorities. (2015, October 1). A Quick Guide to SNAP Eligibility and Benefits. A Quick Guide to SNAP Eligibility and Benefits | Center on Budget and Policy Priorities. Retrieved February 7, 2023, from https://www.cbpp.org/research/food-assistance/a-quick-guide-to-snap-eligibility-and-benefits. Updated January 24, 2023
- Clinical Education. (2022, September 13). Common Nutritional Challenges Within the Older Generation. Common Nutritional Challenges Within the Older Generation | Clinical Education. Retrieved February 7, 2023, from https://www.clinicaleducation.org/resources/reviews/common-nutritional-challenges-within-the-older-generation/
- Flaherty, J. (2017, January 12). Nutrition Challenges as We Age. Retrieved February 7, 2023, from https://now.tufts.edu/2017/01/12/nutrition-challenges-we-age
- Food and Nutrition Service U.S. Department of Agriculture. (2022, August 9). SNAP – Fiscal Year 2023 Cost-of-Living Adjustments. SNAP – Fiscal Year 2023 Cost-of-Living Adjustments | Food and Nutrition Service. Retrieved February 7, 2023, from https://www.fns.usda.gov/snap/fy-2023-cola
- Gabel, K. (2018, March 9). Common Barriers to Senior Nutrition and Tips to Overcome Them. Common Barriers to Senior Nutrition | Advanced Home Health Care. Retrieved February 7, 2023, from https://advanced-homehealthcare.com/common-barriers-to-senior-nutrition-and-tips-to-overcome-them/. Updated November 23, 2021
- Johnson, L., & Saal-Ridpath, K. (2021, September 3). Achieving Nutrition Equity in Older Adults. Achieving Nutrition Equity in Older Adults | ASA Generations. Retrieved February 7, 2023, from https://generations.asaging.org/achieving-nutrition-equity-older-adults
- Kelly, L. (2021, March 26). Consumer Health: Nutrition challenges for seniors. Consumer Health: Nutrition challenges for seniors – Mayo Clinic News Network. Retrieved February 7, 2023, from https://newsnetwork.mayoclinic.org/discussion/consumer-health-nutrition-challenges-for-seniors/
- MacLachlan, M., & Sweitzer, M. (2023, January 25). Summary Findings Food Price Outlook, 2023. USDA ERS – Summary Findings. Retrieved February 7, 2023, from https://www.ers.usda.gov/data-products/food-price-outlook/summary-findings/
- News.iu.edu. (2020, November 16). Senior food insecurity connected to isolation, program barriers in rural areas. Retrieved February 7, 2023, from https://news.iu.edu/live/news/27263-senior-food-insecurity-connected-to-isolation
- Nutrition.gov. (n.d.). Nutrition Programs for Seniors. Nutrition Programs for Seniors | Nutrition.gov. Retrieved February 7, 2023, from https://www.nutrition.gov/topics/food-security-and-access/food-assistance-programs/nutrition-programs-seniors
- Pension Rights Center. (2022, November 28). Income of Today’s Older Adults. Income of Today’s Older Adults – Pension Rights Center. Retrieved February 7, 2023, from https://www.pensionrights.org/resource/income-of-todays-older-adults/. Updated January 30, 2023
- Rodriguez, S. (2022, September 29). Soaring Food Costs Worsen Food Insecurity, SDOH for Older Adults. Retrieved February 7, 2023, from https://patientengagementhit.com/news/soaring-food-costs-worsen-food-insecurity-sdoh-for-older-adults
- Sulo, S., Gramlich, L., Benjamin, J., McCauley, S., Powers, J., Sriram, K., & Mitchell, K. (2020, August 12). Nutrition interventions deliver value in healthcare: Real-world eviden: NDS. Nutrition and Dietary Supplements. Retrieved February 7, 2023, from https://www.dovepress.com/nutrition-interventions-deliver-value-in-healthcare-real-world-evidenc-peer-reviewed-fulltext-article-NDS
- Super User. (2020, August 26). Top 5 Nutritional Challenges for the Elderly. Retrieved February 7, 2023, from https://www.evergreenslc.com/blog/entry/top-5-nutritional-challenges-for-the-elderly
Sweitzer, M., & MacLachlan, M. (n.d.). Retail Food Price Inflation in 2022 surpassed 2021 rates in most categories. USDA ERS – Chart Detail. Retrieved February 13, 2023, from https://www.ers.usda.gov/data-products/chart-gallery/gallery/chart-detail/?chartId=105676. Updated January 26, 2023 - Thornton Snider, J., Linthicum, M. T., Wu, Y., LaVellee, C., Lakdawalla, D. N., Hegazi, R., & Matarese, L. (2014, September 23). Economic burden of community-based disease-associated malnutrition in the United States. Economic burden of community-based disease-associated malnutrition in the United States – PubMed. Retrieved February 7, 2023, from https://pubmed.ncbi.nlm.nih.gov/25249028/
